
Background
Established in 1936 by Geoffrey Lehman, a British missionary surgeon and engineer, Herbertpur Christian Hospital is now a 100 bed multi-speciality hospital which aims to provide quality yet affordable health care to the impoverished communities of rural India.
Main objectives
To broaden my clinical experience by gaining exposure to diseases endemic to rural India, for example tropical illnesses. To explore the health-care challenges faced by a rural missionary hospital in India and how the balance between quality of health-care and affordability works out in reality. To develop my confidence in clinical skills and mature on a personal level by experiencing a new culture.
Main activities
Participating on the ward rounds and out-patient clinics in medicine, general surgery, orthopaedics and ophthalmology. During my surgical attachments, I spent time assisting in operations and any extra time would be spent in the casualty department. Other activities included accompanying hospital staff to rural clinics set up in the neighbouring state of Uttar Pradesh and attending lectures and meetings for post-graduate students and hospital staff respectively.
What I've gained
Clinical Knowledge Having attachments in orthopaedics and ophthalmology was challenging because I had not encountered these specialties before. Examining patients with conditions I had hardly any knowledge of was difficult at first, but by reading up on each disease I have been able to gain clinical knowledge in areas that were once unfamiliar. In orthopaedics for example, examining new patients in the clinic, interpreting their x-rays and assisting in their surgery has deepened my knowledge of fractures and their management. In ophthalmology, learning how to examine patients under the slit lamp with fluorescein dye has enabled me to identify corneal epithelial defects and diagnose conditions such as superficial punctuate keratitis.
During my attachments, I have come across rare congenital abnormalities that have been valuable learning experiences for instance congenital bowing of the tibia, coloboma of the iris and an anencephalic newborn. Gaining exposure to patients with tuberculosis, malaria and enteric fever has taught me how their clinical presentations can often overlap which emphasizes the importance of specific diagnostic tests such as the Widal serological test for enteric fever. I have also learnt about the life-threatening complications of these tropical diseases which can affect multiple organ systems, for example, bowel perforation in enteric fever or myocarditis in malaria. Therefore, clinicians should exercise a high index of suspicion when patients deteriorate in order to detect and treat complications as soon as they arise.
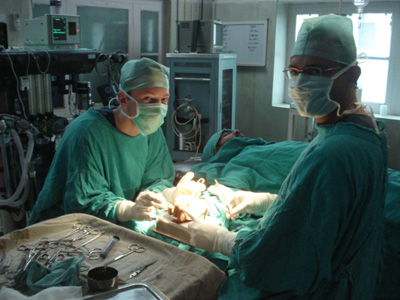
Clinical Skills
In the casualty department, I have taken every opportunity to re-enforce my clinical skills in cannulation, catheterisation, taking ECG's and advanced life-support. It was a nerve-racking experience when I helped assess and treat a girl who had been in a road traffic accident with multiple trauma. It was especially rewarding to develop my suturing skills when I closed one of her scalp lacerations. Assisting a number of times in general, orthopaedic and obstetric surgery has enhanced my ability to maintain an aseptic field and has afforded me opportunities to revise relevant anatomy and hone my suturing technique.
Insights and observations
Aside from the knowledge and skills gained, I have obtained an insight into the difficulties that doctors face when managing very poor patients who have to pay for their treatment. To reduce costs, doctors must be judicious in their use of investigations by extracting pieces of information which dictate treatment and avoiding those which add no benefit to the patient. This is a lesson that will serve me well in my future practice.
Experiencing firsthand how medical practice differs in north India from the U.K. has helped me to appreciate the safe-guards and free health-care we enjoy on the NHS. For instance, I was embarrassed when I had to call back a nurse after she left me alone to take a woman's ECG reading, not aware of the need for a chaperone. I was alarmed when a doctor broke bad news to a man about his dying mother openly in front of other visitors, which has taught me the value of maintaining confidentiality. My empathy for those who cannot afford their treatment has grown when personally faced with the reality of having to pay for my own consultation, investigations and treatment after being struck down by a febrile illness. In a hospital that under-uses analgesia and has no consultant anaesthetist, I squirmed when watching patients endure more pain than would be considered acceptable in the U.K, for instance when a boy had to bare his wound being re-opened and explored with no local anaesthetic. This reminded me of every patient's right to adequate pain relief stipulated by the World Health Organisation.
Quality of teaching experienced
I was fortunate to enjoy the benefits of working in a teaching hospital which included a doctors meeting every morning during which new cases would be discussed, informal teaching during ward-rounds and out-patient clinics and consultant led lectures on topical issues such as cholecystitis, tuberculosis and chronic diarrhoea. Generally speaking, the teaching was of high quality being delivered by experienced clinicians many of whom were experts in their fields. This greatly improved my elective experience.

Opportunities for non-academic activities
Living and working in the same place with the same people for the best part of two months meant that I was able to develop good working relationships with a number of the staff. Consequently, I was fortunate enough to be invited into their homes and have the opportunity to get to know their families. Being in a mission hospital too meant that I had the chance to participate in Christian activities such as Bible studies, times for prayer and worship and Sunday morning church services. Socialising with my work colleagues outside of the hospital environment made me feel part of the community.
Outside of hospital life, I regularly took trips with my friends to the local market place in order to fill ourselves on the popular beef 'mo-mo's' which gave us relief from the bland and repetitive canteen food! At weekends, I made plans to travel to near-by tourist attractions such as Mussorie, a hill station built at 2000m above sea level by the British during the Raj in 1823. Unfortunately, due to the risks of trekking during the tail end of the monsoon season, I decided not to go hiking in the Himalayan foothills.
Problems encountered or unsatisfactory aspects of the attachment
Regarding my attachment, my only complaint is that the doctors and nurses were not readily forthcoming in allowing me to help them. This meant that in order to achieve my aims, I had to be vigilant in seeking out opportunities and be in the right place at the right time. This was often tiring because it required a great deal of motivation and effort. I felt that the staff should have been more aware that being an overseas medical elective student meant that I wanted to gain hands-on clinical experience to make my elective worth-while.
Anything that would have prepared me better
Generally speaking, taking time to arrange non-academic activities before leaving in order to ensure a varied elective experience is a piece of advice I would give to future elective students. Additionally, spending time learning the local language beyond basic phrases will greatly enhance your experience as I can re-call many frustrating times when my basic Hindi still made me dependent upon other people to speak for me. Travelling as light as physically possible will be a huge blessing when walking up endless stairs and hauling luggage onto boats, trains and planes, so only bring what you know you are going to use. Whatever specialties that you work in during your elective, however much knowledge you think you know about it, it will be in your best interest to read up before going in order to get off to a good start with your consultant.
Conclusion
Over-all, this elective from a personal perspective has been an eye-opening and horizon broadening experience with many emotional ups and downs. I have learnt about how radically different Indian health-care and culture is compared to the U.K whilst gaining exposure to a variety of interesting diseases. I have gained confidence and competence in clinical practice considerably and the experience has given me direction for the future.






























