Introduction
My decision to become a doctor stemmed from feeling a call to go abroad, to seek justice for those without a voice, and from feeling medicine would provide me with some sensible skills to do this with. I have always seen my elective period as an opportunity to “test the waters” and therefore arranged a placement through the Emmanuel Hospitals Association in Lakhnadon Christian Hospital, in Madhya Pradesh, India.
Background information
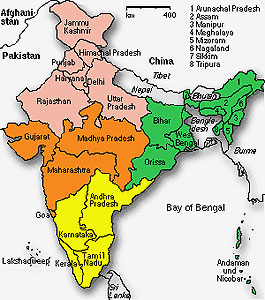
Laknadon Christian Hospital is a small mission hospital in Seoni District in the state of Madhya Pradesh in central India. In the early 1920s, Scottish missionaries seeking to serve the poor of the region set up a clinic, and in the 1970s, a Scottish surgeon further developed the hospital as a surgical unit. There is now also a community HIV project on site.
The 33-bedded hospital has around 2300 patients each year. It has male, female and maternity wards, with several private rooms, and a small nursery, as well as a labour room, operating theatre, small laboratory and X-ray facilities. An acute room facilitates triage, and around 17 000 patients pass through the outpatient department each year. Currently there are 42 staff, with just two full time doctors.
Although Lakhnadon town is relatively wealthy with a large Jain community, the surrounding rural population are mainly tribal subsistence farmers. Fees are charged for all aspects of care, although these may be waived for the poorest patients. Although government healthcare is free, patients still come to Lakhnadon because of the high quality of care offered. Health status is generally poor in the region, with limited access to healthcare facilities. The main burden of disease in the area is infectious diseases.
Devotions were followed by morning ward rounds and any operations, with afternoons spent in the outpatient department, seeing acute admissions and participating in deliveries. The majority of patients were either pregnant women or children. Common presentations included fever and jaundice, and conditions such as malaria, typhoid fever and sickle cell crises were daily occurrences, punctuated by more unusual cases such as snake bites and tetanus. I was also privileged to go to a rural paediatric outreach camp, where we saw many children with scabies and rickets, and sadly one child with marasmus.
The hospital was relatively well equipped, although there were some notable absences, such as a cardiotocograph. The staff had received extensive clinical training; for example, nurses conducted all the spinal anaesthesia. However, the complexities of providing care emerged, often for me echoing lessons from intercalating in International Health. This case illustrates some of the myriad problems facing care provision.
A boy with cerebral malaria
Another afternoon, we were called into the acute room. A bedraggled, malnourished child of around four was unconscious and in status epilepticus. The team took an ABCD approach in an attempt to stabilise him, inserting cannulae and monitoring saturations. His nasogastric tube yielded blood, and as his breathing deteriorated he was intubated, and his mother was instructed to use the bag and mask. After just a couple of hours, he died. It was the first time I have ever taken an active role in an emergency, assisting with the airway management and oxygen, and the images are burned into my memory.
The boy had a 20 day history of fever, but had only been brought to hospital on the twentieth day. His mother had begged her husband to bring him straight to Lakhnadon, but he said that they were too poor to pay hospital fees, and had instead used the little they had to take the child to local quacks and a magician. By that time, the child really needed intensive care of a nature not found anywhere in the region. His arrival in Lakhnadon was realistically a foregone conclusion, and treated by the staff as such. Malaria is a treatable disease, but I learnt that its combination with poverty and gender inequality is lethal.
Reflections
My elective proved an invaluable experience. The most important lesson I learnt was about relying on relationship with God – I was extremely lonely and at times found things very hard. However, by the end, I had gained knowledge, experience and confidence, in addition to a deepened faith. I found living in a completely different culture fascinating, and was privileged to learn about some ofthe complex issues facing the hospital and people of the region.The experience left me with many questions in my mind relating to fair hospital fees, corruption, and equality. It was a wonderful opportunity to have a taster of what I hope to do in the future. I was also reminded afresh of the immense value of even simple research into what lies behind mortality rates, as the deaths I witnessed were all potentially preventable with adequate delineation and amelioration of the inequalities underlying them.
One of my favourite stories from Lakhnadon was that of a woman brought in unconscious with her baby. On arrival at the hospital, her husband was asked to leave the room, and immediately as he departed, the woman sat up on the bed, and explained quietly that her child was sick, but that her husband had refused to bring him to hospital, so she herself had pretended to be seriously ill in order for the child to be brought to the hospital. What an example of love in action!































